Realizing that you or a loved one needs to move into a nursing home can…
In the US, Medicare home health providers, including occupational, speech, and physical therapists, social services, and intermittent skilled nurses, are repeating the same refrain: “Your wife (or partner) is not going to get better, so we have to discontinue our services as Medicare will not pay for it.” Termination of care is swift, often within 48 hours of delivering the message, and the home health care chores fall to the family or must be paid for out of family funds. So what changed?
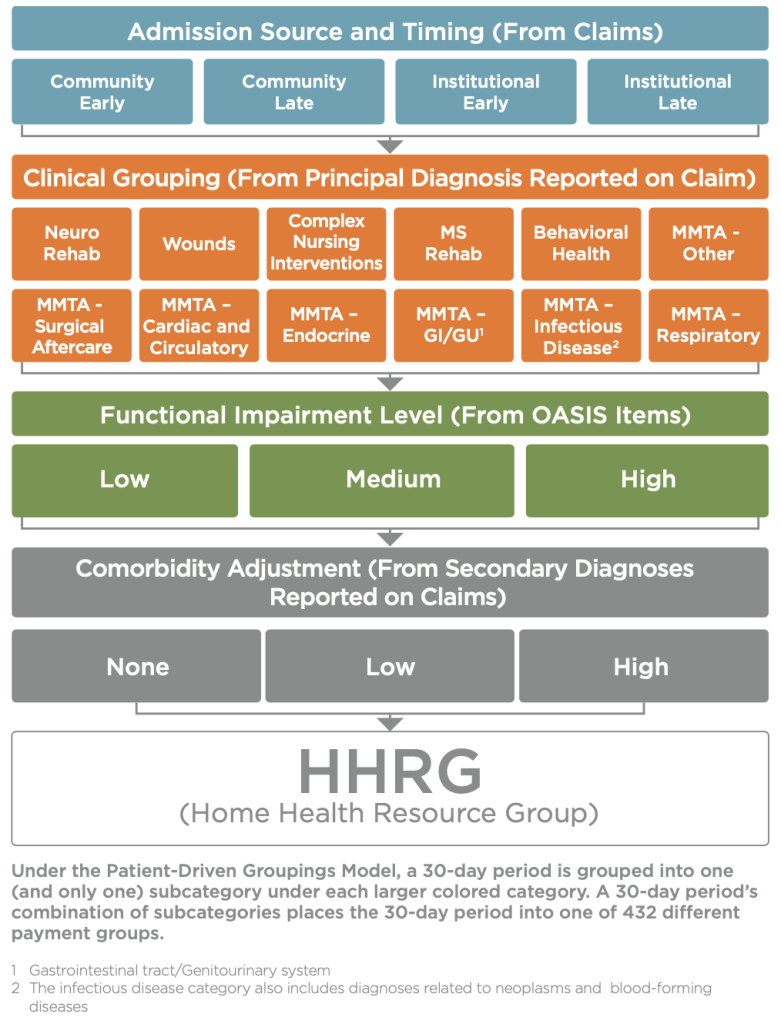
FIGURE 1: STRUCTURE OF THE PATIENT-DRIVEN GROUPINGS MODEL
Significant changes were made in 2020 regarding how Medicare pays for home health services. Medicare altered its billing approach from a therapy-delivered model (the more therapy you receive, the higher the payments billed to Medicare) to a reimbursement system known as the Patient-Driven Groupings Model, or PDGM. Medicare Advantage plans have separate rules and weren’t affected.
How Medicare Categorizes Care and Payment Adjustments
The Centers for Medicare and Medicaid Services (CMS) provide Figure 1 as an example of how a 30-day period becomes categorized into 432 case-mixed groups for adjusting payments in the PDGM. These 30-day periods are further broken into the following subgroups:
- Admission sources and timing
- Twelve clinical principal diagnosis subgroups
- Three functional impairment levels
- Three levels of co-morbidity adjustments
During the 30 days, there is only an allowance for one chosen category under the larger color-coded categories. CMS deems this newer approach to be more holistic regarding patient need assessments.
Before the Medicare Change in 2020
In 2017, the most recent year for which the data is available, for-profit US home healthcare agencies (approximately 12,000) provided care to 3.4 million Medicare beneficiaries. Home
health rates charged were based on the amount of therapy delivered. The more therapy a patient received, the higher the payout to the agency.
CMS believed this new way to assess payments would strike a balance between costs, efficiencies, needs, and outcomes. The members of the National Association for Home Care and Hospice (NAHC) disagreed.
After the Medicare Change in 2020
Due to the change in payment structure, home health care agencies cut back on therapies provided and even reduced the number of therapists employed. They couldn’t bill enough to Medicare to remain profitable. These new payment conditions are based on a patient’s underlying diagnosis and other case-specific complicating medical factors. As a result, home health care agencies now have a stronger financial incentive to meet the needs of short-term therapy, post-hospital or rehab facilities, as well as caring for patients requiring nursing care for complex situations like post-surgical wounds.
CMS looked at the changes in the number of Medicare beneficiaries receiving therapy services due to repricing. They predicted what they would have paid under the old system to what was paid under the new pricing rules using data from actual claims in the PDGM system. The conclusion was that Medicare paid more under the new system and would have to significantly lower home healthcare payments by 2023. Now what?
Look for Advice and Guidance from an Elder Law Attorney
Providing the right patient therapy by home health care agencies at the right time is critical to positive patient outcomes. CMS has done extensive analysis of historical data and, through the use of artificial intelligence tools, feels it can better predict what kind of services and how often a patient will need them through the PDGM. Clarifications are being posted online by CMS that deal with early errors in the program and the ensuing turmoil of therapy provision for patients within the new guidelines. Hopefully, more reviews and revisions to the PDGM will strike a better balance between cost and efficiency, patient therapy needs, and outcomes.
Understanding the role Medicare plays in long-term care services can be confusing. We help families plan for the possibility of needing long-term care and how it could be paid for without placing the burden on family members. Please contact our law firm to speak with a qualified elder law and estate planning attorney to tailor a long-term care protection plan for you or your loved one. We look forward to the opportunity to work with you.


Comments (0)